What to expect at your consultation
A clear starting point for TMS therapy
If you’re exploring TMS therapy for depression, anxiety, PTSD or another complex condition, the first step is a consultation.
This ensures clinically appropriate care and helps answer the practical questions early: whether transcranial magnetic stimulation may be appropriate for you, what the process involves, what treatment may cost, and what happens next.
Every consultation sits within a psychiatrist-led model of care, with clear communication back to your GP or treating practitioner if you so wish.
Ready to get started?
How the consultation process works
Starting TMS begins with assessment, review and a clear understanding of your history.
1. Referral and initial contact
To begin, you will usually need a referral from your GP or psychiatrist.
Once we receive your referral, our team will:
- contact you to arrange an initial phone screening
- gather relevant background information
- explain the next steps
- answer early questions about eligibility, timing and funding.
This stage helps us understand your situation before your psychiatric assessment.
2. Psychiatric assessment
Before treatment begins, you’ll have a session with our psychiatrist, who may wish to know about:
- your mental health history
- previous treatment approaches, including medication and therapy
- your current symptoms.
This session enables the psychiatrist to determine if TMS treatment is clinically appropriate for you (not everyone is suitable).
For many, there is a $220 out-of-pocket fee for a psychiatrist assessment.
3. Treatment planning
If TMS therapy for depression or another condition is considered appropriate, we develop a treatment plan around your clinical needs.
Your plan may outline:
- the recommended course of treatment
- session frequency
- review points during treatment
- communication with your GP or other treating practitioners.
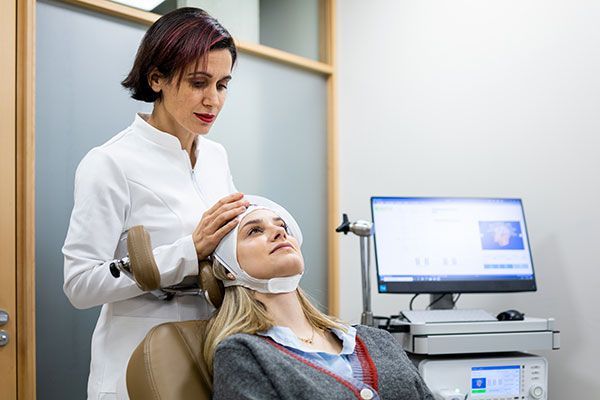
What to expect at your appointment
TMS is delivered in-clinic at our Margate and Caboolture locations.
A typical session:
- takes around 20 to 30 minutes
- is completed while you are awake and seated comfortably
- does not involve anaesthesia
- does not require recovery time afterwards.
We encourage you to personalise your session with your choice of playlist. Our goal is to ensure you feel calm and comfortable during your treatment.
What does TMS treatment feel like?
Hopefully, quite comfortable. Many people describe a tapping or clicking sensation during treatment.
Please tell us if anything feels too much, as we can adjust the settings to improve your comfort.
Conditions TMS may support
While the strongest clinical evidence for TMS relates to depression, TMS may also be considered, under psychiatric guidance, for individuals diagnosed with other conditions.

- Post-traumatic stress disorder (PTSD)
- Anxiety disorders
- Obsessive compulsive disorder (OCD)
- Chronic pain conditions
- Addiction and substance use disorders
- Insomnia
- Tinnitus.
Research into these applications continues to evolve. For many of these conditions, TMS may be used as part of a broader treatment plan rather than a standalone intervention.
Suitability is determined on an individual basis following a comprehensive psychiatric assessment.
Costs and funding
Cost is one of the first questions many people ask, and we understand why.
Have been diagnosed with depression, anxiety, PTSD, or another psychiatric condition
Have tried medications and psychological therapy without sufficient relief (treatment-resistant depression)
Can’t take medications due to side effects or prefer not to take medication
All treatment decisions are made on an individual basis and guided by clinical judgement.
Alata
Alice
Open Sans
Noto Sans
Bebas Neue
Great Vibes
Rock Salt
Exo
Belgrano
Overlock
Cinzel
Indie Flower
Staatliches
Roboto Slab
Lato
Noto Serif
Open Sans
Montserrat
Ubuntu
Rubik
Delius
Amiri
Montserrat
A structured, clinician-led approach
Connected Minds TMS operates with a strong emphasis on governance, care protocols, and communication across treatment teams.
Our model includes:
- Psychiatrist-led assessments
- Individualised treatment planning
- Regular progress reviews
- Clear documentation and GP updates
- Coordination with your existing mental health providers
This approach supports continuity of care and informed decision-making.
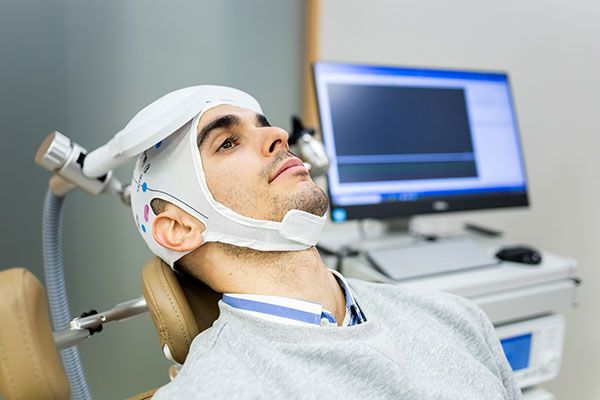
What to expect from the treatment process
While treatment plans vary, TMS therapy typically involves:
- An initial psychiatric consultation
- A course of scheduled sessions delivered over several weeks
- Ongoing monitoring and review

Information for referring doctors
Connected Minds welcomes referrals from clinical partners.
We provide:
- Clear referral pathways
- Timely assessment availability
- Written correspondence and progress updates
- A collaborative, shared-care model.
Referrals may be appropriate where patients require specialist assessment for advanced treatment options within a psychiatric framework.
Funding and accessibility
Medicare
TMS may be covered under the Medicare Benefits Scheme (MBS) for eligible patients who meet clinical criteria. In many cases, the initial course of treatment is bulk billed, with additional sessions available under Medicare if required.
WorkCover and DVA
TMS treatment may also be funded through WorkCover or the Department of Veterans’ Affairs (DVA), subject to approval and eligibility criteria. Our team can assist with documentation and coordination where applicable.
Privately funded sessions
Private sessions are available for patients who are not eligible for Medicare or third-party funding.
Serving north Brisbane from Margate and Caboolture
Connected Minds services patients across Margate, Caboolture and the north Brisbane region, offering access to TMS therapy in a friendly local clinic.
Enquire today
Please contact us to request further information or arrange an initial assessment.

Frequently asked questions
How long does TMS treatment take?
Each session usually lasts around 20–40 minutes. A full course of treatment may involve 35 sessions over several weeks, with additional maintenance sessions available depending on your treatment plan.
Is TMS painful?
TMS is not usually described as painful. Some people experience a tapping or clicking sensation on the scalp and you may feel mild discomfort as you get used to the stimulation.
If you feel uncomfortable at any point, please tell us and we will adjust your treatment.
Is TMS covered by Medicare?
Yes, if you meet the government’s eligibility criteria and clinical requirements.
We provide TMS treatment for an initial 35 sessions, which (in most cases) will be bulk billed under the Medicare Benefits Scheme (MBS). If maintenance TMS treatment is required, the MBS will also cover a further 15 sessions after 4 months.
We offer low-cost private sessions for patients who are not eligible for Medicare funding.
Does TMS affect memory?
TMS is not usually associated with memory loss. It does not involve sedation or seizure induction, and you remain awake and alert throughout treatment.
If you have any questions or concerns about cognitive effects, please discuss them with us before commencing treatment.

